Have you ever wondered how those pruney fingers happen when you are in the pool or the bath for a while?
Or ever wondered what purpose they serve?
Until recently I had no idea how or why it happens. To be honest, I hadn’t given it much thought.
You might also wonder what this has to do with the title about neurodynamics and nerve testing.
Well, let me explain …
Why are pruney fingertips (and feet) useful?
I had never given any thought to why our fingers and toes prune up, beyond being an indication that you had been in the water for a long time.
It turns out that these wrinkly digits may actually serve a functional purpose.
Researchers believe that this phenomenon may have evolved to enhance our grip on wet objects or surfaces.
In 2011, an experiment showed that wrinkled fingers performed significantly better with manipulating wet marbles than doing the same task with dry, unaltered fingers.
The theory was that the wrinkles act as tiny channels, allowing water to drain away and improving the contact between the fingertips and wet surfaces.
You can think of it like how tyre tread allows the tyre to grip the road better in the wet, as opposed to slick tyres.
In 2020, a sample of 500 volunteers were able to show that the wrinkling increased the friction between fingers and a plastic object, meaning that less effort was required to grip.
This could be incredibly useful if you were operating with wet hands on wet objects.
Interesting fact
It takes females longer to develop pruney fingers than males.
Why? No idea!
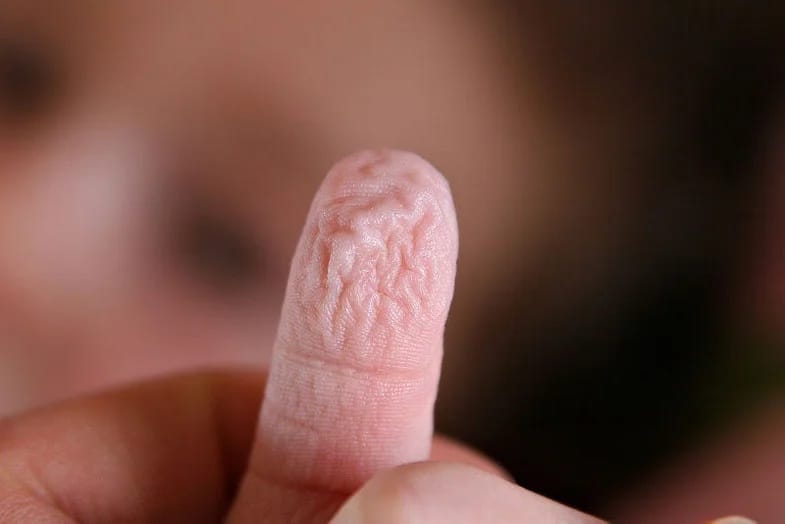
How do pruney, wrinkly fingers happen?
I had always thought that these wrinkly fingers were just caused by the skin softening and perhaps absorbing some water.
There is evidence that the outer layers of skin may swell a little from being in water, but that isn’t the only mechanism involved.
If it were down to osmosis alone, our skin would need to swell by 10% to achieve the wrinkles we see in our fingers, leaving them even more hilariously enlarged than the digits of our head of Commonwealth.
It turns out that the wrinkling of fingers and toes in water is a response controlled by our sympathetic nervous system.
What Is The Sympathetic Nervous System?
Your sympathetic nervous system is one half of your autonomic or ‘automatic’ nervous system. The sympathetic nervous system is responsible for the ‘fight, flight and fright’ response.
(The other half is the parasympathetic nervous system, which literally means ‘alongside’ your sympathetic nervous system. The parasympathetic nervous system comes into its own when you are resting and digesting.)
The autonomic nervous system controls involuntary bodily functions, including heart rate, blood pressure and the constriction and dilation of blood vessels (and lots of other things!)
Since the 1930s, scientists have suspected that the nervous system had something to do with these pruney fingers.
When they assessed patients with median nerve injuries (one of the main nerves to the hand) they didn’t develop the same wrinkly fingers!
It seems that when immersed in water, there is some kind of signalling to the blood vessels in our extremities to constrict.
What generates that signalling is not known for sure, however there might be a clue in this interesting fact: finger tip wrinkling takes longer to happen in saltwater.
Our current understanding of pruney fingers
The most recent thinking is that water does penetrate the outer skin layer, causing the outermost cells to swell slightly.
Alongside that, there is a sympathetic nervous system response that causes blood vessel constriction.
The combination of constricted blood vessels and swollen outer cells creates tension on the skin’s surface, leading to the formation of wrinkles.

In the 1970s, the wrinkly finger phenomenon lead to doctors proposing a simple bedside test to test for nerve damage involving immersing the hand in water.
This was especially useful for assessing unconscious patients.
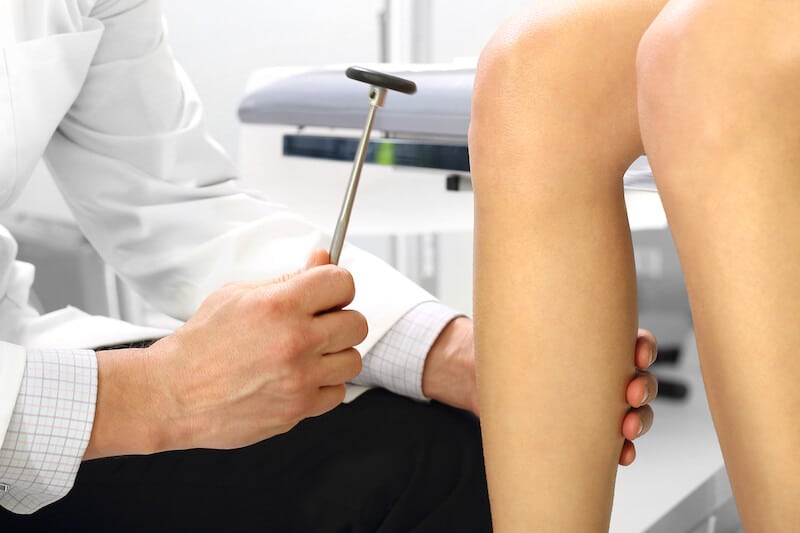
How do you test nerves?
Your health professional has a number of ways of testing nerve conduction in the clinic. They can test your
- deep tendon reflexes
- light touch sensation
- proprioception (joint position sense)
- strength
- vibration detection
Nerve conduction tests are another tool, but have limitations and the drawback of not being able to be done in the clinic by a physio or a GP and require special equipment and knowledge.
The pruney finger test isn’t part of the normal nerve-testing repertoire.
However, none of these test a key element of nerve health.
What are neurodynamic tests?
Why do we need them?
The other aspect of nerve health which needs to be tested is its more physical properties.
A nerve needs to be able to slide, glide and cope with sometimes amazing changes in length and the path that they travel, but still conduct.
Consider activities like dance, fast bowling, or gymnastics.
It is incredible to see all the different positions and the extremes that a nerve needs to be able cope with and still conduct faultlessly to allow messaging to and from the central nervous system.
And this isn’t even considering the conduction of the autonomic nervous system, which is not as immediately obvious.
When do neurodynamic tests get used?
Neurodynamic tests are commonly used by doctors and physio when they are assessing musculoskeletal pain problems.
The base neurodynamic tests include:
- upper limb neurodynamic test
- straight leg raise
- slump test
- prone knee bend
- passive neck flexion
Each of these neurodynamic tests have ways they can be customised to explore different problems.
For example, you can bias a straight leg raise or a slump test differently to explore pain on the outside of the foot versus the top of the foot versus the inside of the foot versus the heel.
With upper limb problems, you would use a different bias of the upper limb neurodynamic test to assess a tennis elbow type pain compared to a carpal tunnel syndrome type pain.
All of these tests are standard for our physiotherapists in a complete assessment of a painful condition.
Learn more about our physiotherapy services here.
What do neurodynamic tests assess?
Neurodynamic tests are used to test the physical properties and the physical health of nerves.
Neurodynamic testing assesses:
- how a nerve copes with movement
- how it copes with the demands of more tension on it
- how a nerve moves and glides in relation to its interfaces along its path
Importantly, they are also a test of sensitivity of the neuroimmune system.
In the past, they have been at times misunderstood and misused to look at ‘nerve tightness’ and used as some kind of ‘nerve stretch’.
The term neural tension has been dropped in favour of the term neurodynamics as it is better reflects what the tests are for.
We are testing the physical properties of not just the peripheral nerves but spinal cord and meninges, including how they move, how they glide and slide, if they are sensitive and if their ‘messaging’ is altered.
Here is Dr David Butler demonstrating some of the concepts of neurodynamics. He literally wrote the book – it is a classic called ‘Mobilisation Of The Nervous System’.
What symptoms do we expect with neurodynamic tests?
The kind of symptoms that we commonly look for are
- the reproduction of the person’s pain
- sensations of tightness or pins and needles
- restriction of movement
However there are more subtle symptoms that can be provoked like skin colour changes, sweating and – as I found out recently – pruney fingers.
I have never thought to take note of fingertip skin wrinkling as a possible sign of altered neurodynamic function and altered sympathetic function.
However, knowing that this is underpinned by the sympathetic nervous system function, it makes sense to consider these signs when doing any neurodynamic testing.
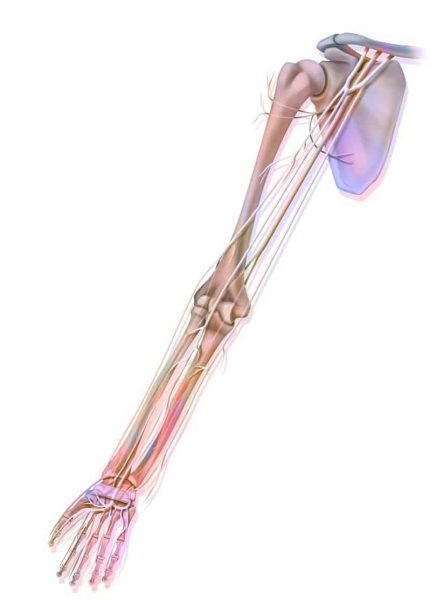
'It's my hand, not my neck!'
When someone comes in to a get help from a physio for arm pain, it is important to first work out is whether there is something related to the neck that is causing the arm pain.
Even when it ‘seems’ obvious that it is a shoulder, elbow, wrist or hand problem, it is incredibly common to find that there is something relevant in the person’s neck.
The EXPOSS study looked at the frequency of limb pain of spinal origin, even when the patient and referring doctor DO NOT think that it is of spinal origin.
They studied 369 participants who had isolated extremity (arm or leg) pain and did not believe that it originated from the spine.
More than 40% of them responded to spinal intervention and had a better outcome than those who were found to be a true extremity problem.
This study was fascinating in showing how often the spine is the true source of extremity pain.
It happens a lot!
Pruney fingers - a case study
A gentleman recently came in complaining of significant arm pain on both sides, particularly in both hands.
We went about checking the usual things – neck function, upper limb movement and strength, neurological function, positions and movements that reproduce the pain.
He commented that when his pain was present, he had wrinkling on his finger tips, as if they had been wet too long.
Sure enough, when I asked him to perform a movement that reproduced his pain, he started developing pruney fingers right before my eyes!
When we performed all the variations of the upper limb neurodynamics, they were all positive and similarly changed his finger tip skin.
These findings didn’t make sense to me until I learnt that the skin wrinkling is a function of the sympathetic nervous system, and this was a sign of altered sympathetic function.
It underlined to me that upper limb neurodynamic testing continues to be important, and that sympathetic responses need to be checked in everyone.
Summary
Finger (and toe) wrinkling and the prune-like appearance is driven by a sympathetic nervous system response. It is not due to swelling or osmosis.
A pruney finger response to neurodynamic testing is another sign of altered neural function.
Neurodynamic testing is used for testing the physical properties of the neuroimmune system.
It is indispensable because it tests for aspects of nerve function that cannot be tested with other neurological tests.
Other articles that might be of interest:
Physiotherapy – Assessing neurodynamics is one part of a comprehensive assessment of your problem.
Persistent pain – We have an interest in helping persistent pain, and neurodynamics can be a common contributor that is overlooked.
Plantar fasciitis – Heel pain is commonly diagnosed as plantar fasciitis without considering if there is a neural element that needs to be addressed (and can improve quickly when it is!).